- Visibility 58 Views
- Downloads 9 Downloads
- DOI 10.18231/j.ijor.2021.011
-
CrossMark
- Citation
Bilateral idiopathic club foot in baby of a rheumatoid mother: A rare case report and its management
- Author Details:
-
Alok Chandra Agrawal
-
Anupam Pradip Inamdar
-
Ranjeet Choudhary *
-
Pandya Raj
-
Shilp Verma
Introduction
Congenital talipes equinovarus or congenital clubfoot is the most common congenital orthopedic condition requiring intensive treatment. It is characterized by forefoot adduction, mid-foot cavus, heel varus, and ankle equinus.[1], [2] It is caused by congenital abnormalities of multiple musculoskeletal tissues distal to the knee (musculotendinous, ligamentous, osteoarticular, and neurovascular structures).[2], [3], [4] It has a multifaceted etiology, with several hypotheses offered in its etiopathogenesis, including an in-utero mechanical block, a primary germ-plasm defect in the talus, myofibroblast contraction leading to retraction fibrosis neurogenic, myogenic, and vascular theories.[5] The incidence of congenital clubfoot in the general population is 1 to 2 in 1000 live births.[6] During pregnancy, rheumatoid arthritis has a more favorable prognosis and requires fewer immunomodulatory drugs to maintain disease activity levels. The majority of women experience flare-ups during the postpartum period and the requirement of immunomodulator is increased.[7], [8] Children born to RA mothers have been reported to be healthier and have a higher mean birth weight than children born to nonrheumatic mothers if they are in remission.[9] A higher risk for congenital abnormalities in the offspring of pregnant women with RA was not found. Thus, contrary to popular belief, RA has a favorable effect not just on pregnant mothers, but also on their fetuses.[9] However, clubfoot has rarely been reported in babies born to women who have rheumatoid arthritis (RA). We present a rare case of a 31-year-old lady with RA on disease-modifying anti-rheumatoid drugs who delivered a child with bilateral idiopathic clubfoot.
Case Report
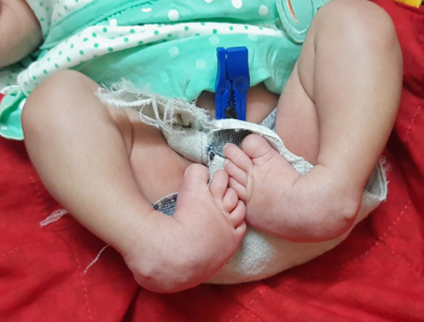
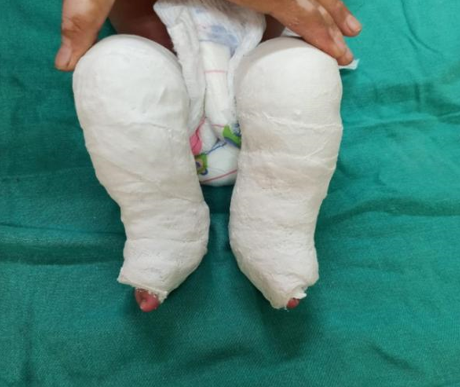
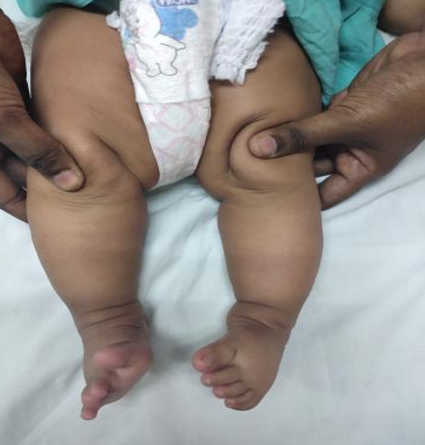
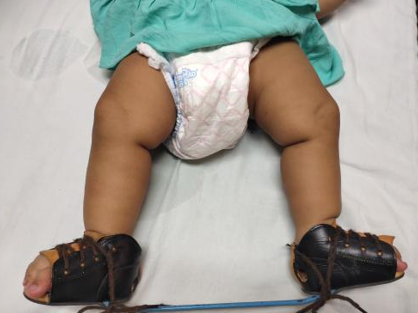
A two-week-old girl born in a non-consanguineous marriage to a 31-year-old mother with RA presented to us with bilateral ankle and foot deformities. The mother had a history of rheumatoid arthritis diagnosed at seventeen years of age. She is being treated with disease-modifying anti-rheumatoid drugs (DMARD) since 2012. Her DMARD regimen was begun with Injection Tocilizumab 400mg administered four weeks apart for six months, followed by oral Methotrexate, Hydroxychloroquine, and Sulfasalazine. She underwent a total knee arthroplasty of the right side in September 2019. Methotrexate was discontinued seven months before the conception. However, Hydroxychloroquine and Sulfasalazine tablets were continued in all three trimesters of pregnancy. She received regular Folic acid supplementation before conception and during the pregnancy. A full-term female baby was delivered by cesarean section. APGAR score was eight on ten at one and five minutes, and baby weight at birth was 3 kilograms. On examination, the child had normal reflexes, was accepting feed normally, and there were no cyanotic spells. The vitals, oxygen saturation, urine output, and systemic examination were normal. The upper to lower segment ratio was normal. There were no signs of spinal dysraphism, and neurofibromatosis. The upper extremities were normal. Both ankles and feet were in an abnormal position, with forefoot adduction and pronation, cavus in the midfoot, heel varus in the hindfoot, and equinus in the ankle joints, indicating a bilateral clubfoot deformity. The clubfoot deformities were evaluated with the modified Pirani score, which was scored eight out of ten (Figure 2). The deformity correction was begun at two weeks of age by the Ponseti serial casting method. The Ponseti casts were changed at weekly intervals (figure 3). The forefoot adduction and heel varus deformities were corrected in five Ponseti casts. The equinus deformity was treated with Botox injections, followed by an above-knee cast with the ankle in neutral dorsiflexion for one week, then 20 degrees dorsiflexion for two weeks. Following deformity correction, the final modified Pirani score was two out of ten (Figure 3). For three months, a foot abduction brace was worn for 23 hours per day to keep the deformity corrected, after which it was only worn at night and during naps (figure 4). The child has normal developmental milestones and is thriving well. The mother has achieved sustained remission in RA.
Discussion
RA, a chronic autoimmune inflammatory disease with significant physical impairment, affects women three times as many as men, often in childbearing years.[7], [10] Pregnancy hormones, such as progesterone suppress the immune relationship between the mother and the fetus by modulating Th1/Th2 cytokine balance, resulting in a favorable pattern of RA in pregnancy.[11], [12], [13] Pregnancy's complex hormonal and immunological changes may have an impact on rheumatoid arthritis immunoregulation. Some studies have suggested that decreased interferon-gamma production and an imbalance in interleukin six and interleukin 12 production are to cause RA remission during pregnancy. [14] The maternal immune response to fetal paternally acquired class II HLA antigens, CD8+ and CD4+ T cells, placental gamma globulins, and alterations in serum fetal DNA levels (trophoblast generated) may also play a significant role in pregnancy-induced RA remission.[15], [16] The effect of RA on fetuses in a pregnant woman is less well understood, with scant evidence on the risk of structural limb abnormalities.Although pregnancies with RA have not been linked to an increased risk of congenital anomalies in the fetus,anomalies, undescended testis, polydactyly, and syndactyly in rheumatoid arthritis fetus as in the general population. The clubfoot has rarely been reported.[9] A higher incidence of musculoskeletal deformities in Hydroxychloroquine administered rheumatoid mothers has been shown. However, the type of anomaly has not been specified. Hence, we are reporting this rare case of bilateral clubfoot in RA's mother.[17] Ventricular septal defects and coarctation of the aorta have been described in babies born to mothers who have received sulfasalazine during pregnancy. However, musculoskeletal abnormalities have not yet been reported as their teratogenicity. [18] This infant was exposed to Sulfasalazine throughout pregnancy (500 mg two times a day)
The most common age group for rheumatoid arthritis in Indian women is between the ages of 35 and 45 years, [19] while the median age at first pregnancy among married women in India is 21 years.[20] Thus, RA occurs in a later age group, which might be one of the probable explanations for the low incidence of clubfoot in babies born to RA mothers. The standard treatment of choice for idiopathic clubfoot is the Ponseti serial casting method, which consists of two distinct stages of manipulation and maintenance. The manipulation phase includes using the talus head as a fulcrum, supinating the forefoot with pressure on the first metatarsal to eliminate the cavus deformity, and then abducting the forefoot. This is followed by the application of a plaster cast, which holds the foot in the correct position and allows enough time for soft tissue remodeling. It is repeated weekly for an average of 5-6 weeks until the abduction of the forefoot is reached by 50 degrees. The equinus deformity must be corrected by serially stretching the tendoachilles to achieve dorsiflexion of the ankle joint and lengthening the tendoachilles with a tenotomy or Botox injection in resistant cases. It is then followed by three weeks in a supporting cast to aid in healing the lengthened position. During the maintenance phase, the foot is kept in an abduction brace for 23 hours per day, reducing recurrence rates. [21] We successfully corrected clubbed foot deformity in a baby of a rheumatoid arthritis mother using the Ponseti serial casting method. Our findings validate the Ponseti serial casting method for these kinds of patients.
Conclusion
Bilateral clubfoot in babies born to rheumatoid mothers is a rare presentation. It can be successfully treated with serial Ponseti corrective casts similar to idiopathic clubfoot in babies born to non-rheumatoid mothers.
Source of Funding
No financial support was received for the work within this manuscript.
Conflict of Interest
The authors declare they have no conflict of interest.
References
- E Ippolito, I V Ponseti. Congenital club foot in the human fetus. A histological study. J Bone Joint Surg Am 1980. [Google Scholar]
- A Anand, DA Sala. Clubfoot: Etiology and treatment. Indian J Orthopaedics 2008. [Google Scholar] [Crossref]
- H Isaacs, JE Handelsman, M Badenhorst, A Pickering. The muscles in club foot--a histological histochemical and electron microscopic study. J Bone Joint Surg Br 1977. [Google Scholar] [Crossref]
- V Ionasescu, J A Maynard, I V Ponseti, H Zellweger. The role of collagen in the pathogenesis of idiopathic clubfoot. Biochemical and electron microscopic correlations. Helv Paediatr Acta 1974. [Google Scholar]
- V Pavone, E Chisari, A Vescio, L Lucenti, G Sessa, G Testa. The etiology of idiopathic congenital talipes equinovarus: a systematic review. J Orthop Surg 2018. [Google Scholar]
- G Biruly, NK Karsh, N Panchbhai, K Satyam, D Kumar, D Kumar. Socio-demographic characteristics of clubfoot patients: An observational study. Int J Orthop Sci 2020. [Google Scholar] [Crossref]
- R Partlett, E Roussou. The treatment of rheumatoid arthritis during pregnancy. Rheumatol Int 2011. [Google Scholar] [Crossref]
- A Makol, K Wright, S Amin. Rheumatoid arthritis and pregnancy: safety considerations in pharmacological management. Drugs 2011. [Google Scholar]
- É Pósfai, F Bánhidy, R Urbán, A E Czeizel. Birth Outcomes of Children Born to Women with Rheumatoid Arthritis. Cent Eur J Public Health 2015. [Google Scholar]
- A Florea, C Job-Deslandre. Polyathrite rhumatoïde et grossesse. Presse Med 2008. [Google Scholar] [Crossref]
- J W Bijlsma, O Huber-Bruning, J H Thijssen. Effect of oestrogen treatment on clinical and laboratory manifestations of rheumatoid arthritis.. Ann Rheum Dis 1987. [Google Scholar] [Crossref]
- J Dulos, P Vijn, C van Doorn, CL Hofstra, D Veening-Griffioen, J de Graaf. Suppression of the inflammatory response in experimental arthritis is mediated via estrogen receptor α but not estrogen receptor β. Arthritis Res Ther 2010. [Google Scholar] [Crossref]
- RL Wilder. Hormones, Pregnancy, and Autoimmune Diseases. Ann N Y Acad Sci 1998. [Google Scholar] [Crossref]
- H Tchórzewski, G Krasomski, L Biesiada, E Glowacka, M Banasik, P Lewkowicz. IL-12, IL-6 and IFN-γ production by lymphocytes of pregnant women with rheumatoid arthritis remission during pregnancy. Mediators Inflamm 2000. [Google Scholar] [Crossref]
- SH Zrour, R Boumiza, N Sakly, R Mannai, W Korbaa, M Younes. The impact of pregnancy on rheumatoid arthritis outcome: The role of maternofetal HLA class II disparity. Joint Bone Spine 2010. [Google Scholar] [Crossref]
- M Ostensen. Sex Hormones and Pregnancy in Rheumatoid Arthritis and Systemic Lupus Erythematosus. Ann N Y Acad Sci 1999. [Google Scholar] [Crossref]
- K F Huybrechts, B T Bateman, Y Zhu, L Straub, H Mogun, S C Kim. Hydroxychloroquine early in pregnancy and risk of birth defects. Am J Obstet Gynecol 2021. [Google Scholar]
- J J Hoo, T A Hadro, P Von Behren, . Possible teratogenicity of sulfasalazine. N Engl J Med 1988. [Google Scholar]
- S Pati, K C Sahoo, M Samal, S Jena, P Mahapatra, D Sutar. Care-seeking pathways, care challenges, and coping experiences of rural women living with rheumatoid arthritis in Odisha, India. Prim Health Care Res Dev 2019. [Google Scholar]
- . India - median age at first pregnancy by age groups 2016 [Internet]. Statista. [cited 2021 May 27]. . [Google Scholar]
- M Kadhum, L Mu-Huan, J Czernuszka, C Lavy. An Analysis of the Mechanical Properties of the Ponseti Method in Clubfoot Treatment. Appl Bionics Biomech 2019. [Google Scholar] [Crossref]
